A study by Oxford orthopaedic researchers has found that hip replacements using cement improved the quality of life of patients, compared to uncemented implants.
The findings of the White 5 trial, which is supported by the NIHR Oxford Biomedical Research Centre (BRC), have been published in the New England Journal of Medicine.
Hip fracture in older people is a global problem that negatively affect patients’ quality of life and places a burden on healthcare systems. In the UK there are about 70,000 hip fractures every year, and each is a potentially catastrophic event; approximately 20 per cent of patients will die during the first year following the injury, and those who survive suffer pain and lack of mobility.
“About half of all hip fractures happen at the neck of the femur, or thighbone,” said Matt Costa, Professor of Orthopaedic Trauma at NDORMS, and Co-theme Lead of the Oxford BRC’s Musculoskeletal Theme.
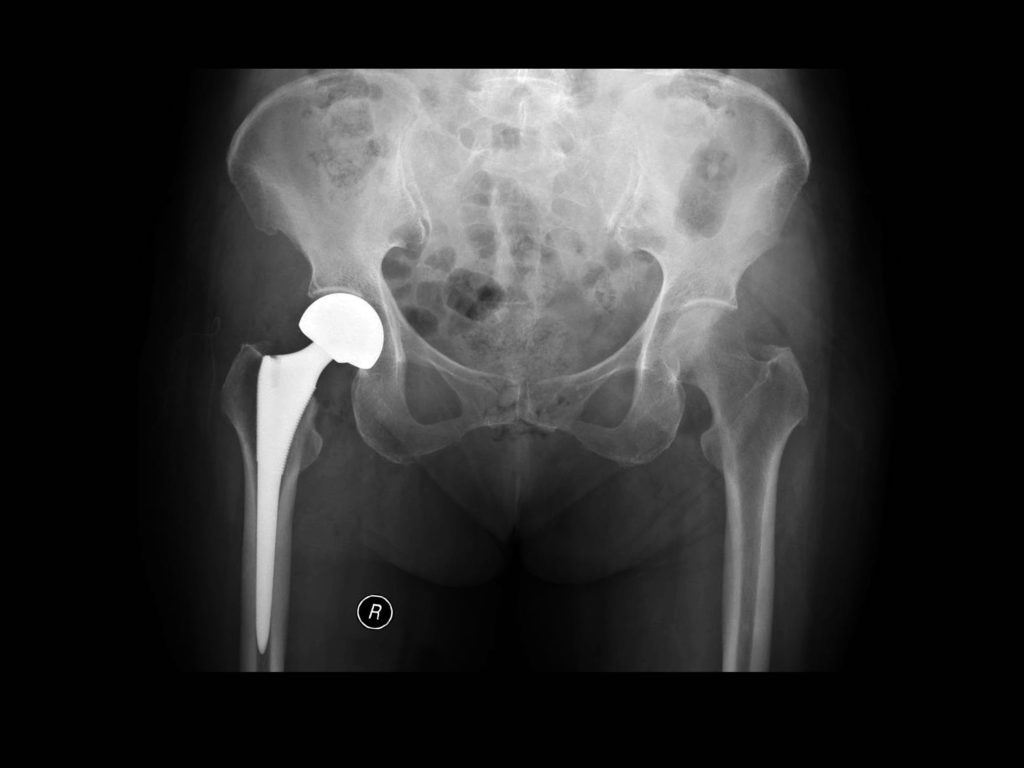
“These are treated with a hip replacement procedure called hemiarthroplasty, in which the head of the femur is replaced with a metal implant. The most common method to fix the implant in place has been to use cement bonded to the patient’s bone but this isn’t without its risks during surgery. New implants have been designed without cement, so we set up the White 5 trial to compare any difference between the treatments and the effect on patient outcomes.”
The challenge with fixing implants to the bone is that they can loosen if not bonded securely to the patient’s thighbone, causing pain and restricting day-to-day activities. Bone cement provides reliable bonding to the bone but there is a small risk that a patient’s blood pressure may drop as the cement is injected into the bone.
The newer uncemented implants have been designed to provide better integration with the bone and are claimed to provide reliable fixation and an early return to normal activities, without the risks of bone cement.
The White 5 trial, a randomised controlled trial across multiple hospitals in the UK, recruited people over the age of 60 with a hip fracture requiring hemiarthroplasty: 610 patients were recruited to receive the cemented treatment, and 615 to the modern uncemented treatment.
The study found that patients having the cemented treatment showed a statistically significant improvement in quality of life at one month and four months after the procedure, although there was less difference after 12 months.
Secondary fractures at the site of the implant were more common in the uncemented than cemented group. There was no difference between the two groups in terms of the number of people who died.

Professor Costa (pictured left) said: “Cemented implants provide modest but important improvements in quality of life compared with uncemented implants. The cemented implants also reduce costs for the NHS. Overall, we would recommend clinicians use cemented implants for patients having a hemiarthroplasty for their hip fracture.”
The involvement of patients and the public in trials to advance research and treatments can’t be underestimated.
Alwin McGibbon got involved 15 years ago: “Back when I joined, hospitals generally each had their own outcome measures, so it was like comparing apples and pears because they would have a different set of questions. I’ve been involved in White 5 on and off since it started, and part of my PPI (patient and public involvement) work was to develop the outcome measures for the trial, which have been now adopted by most of the hospitals.”
Alwin played a key role in patient-facing activities, such as putting documentation like consent forms into plain English.
“It’s nice to see the whole thing through from the beginning and knowing that you’re making a difference for patients,” she said.
